 Background: In the UK, there are over 16,000 new cases of rectal cancer per year. Treatment includes chemotherapy and radiotherapy, followed by major surgery, especially in those patients deemed as ‘high-risk’. There are risks of surgical complications, long-term side-effects, and about a third of patients require a permanent colostomy (a ‘bag’).
Background: In the UK, there are over 16,000 new cases of rectal cancer per year. Treatment includes chemotherapy and radiotherapy, followed by major surgery, especially in those patients deemed as ‘high-risk’. There are risks of surgical complications, long-term side-effects, and about a third of patients require a permanent colostomy (a ‘bag’).
In the past 5-8 years, researchers have found that rectal tumours may totally disappear after chemo-radiotherapy in 25% patients (known as a clinical complete response), avoiding the need for surgery. This is a new type of rectal cancer management known as ‘organ preservation’. Instead of surgery, patients are actively monitored, ‘watch-and-wait’, to ensure tumours have not returned.
Initially, doctors were nervous that not giving patients surgery might compromise long-term survival. However, one of the largest studies in the world addressing this question and based in NW England (the OnCoRe project; lead: Renehan), showed that this approach is safe.
There is a common perception among cancer doctors that organ preservation is a good thing, but there is little research addressing patient preferences. Specifically, no research has investigated how people balance the characteristics of these treatments and make decisions.
Methods: Over 2 years, we will undertake two levels of research. First, an online survey to understand preferences for (i) surgery alone versus chemo-radiotherapy plus surgery; and (ii) where tumours disappear after chemo-radiotherapy, the options of watch-&-wait versus surgery by presenting hypothetical treatment scenarios, described by their characteristics, to 100 patients and 100 public participants – accessed through internet providers and charities.
Second, we will translate the survey information to build a web-based decision aid, known as “DCIDA”.
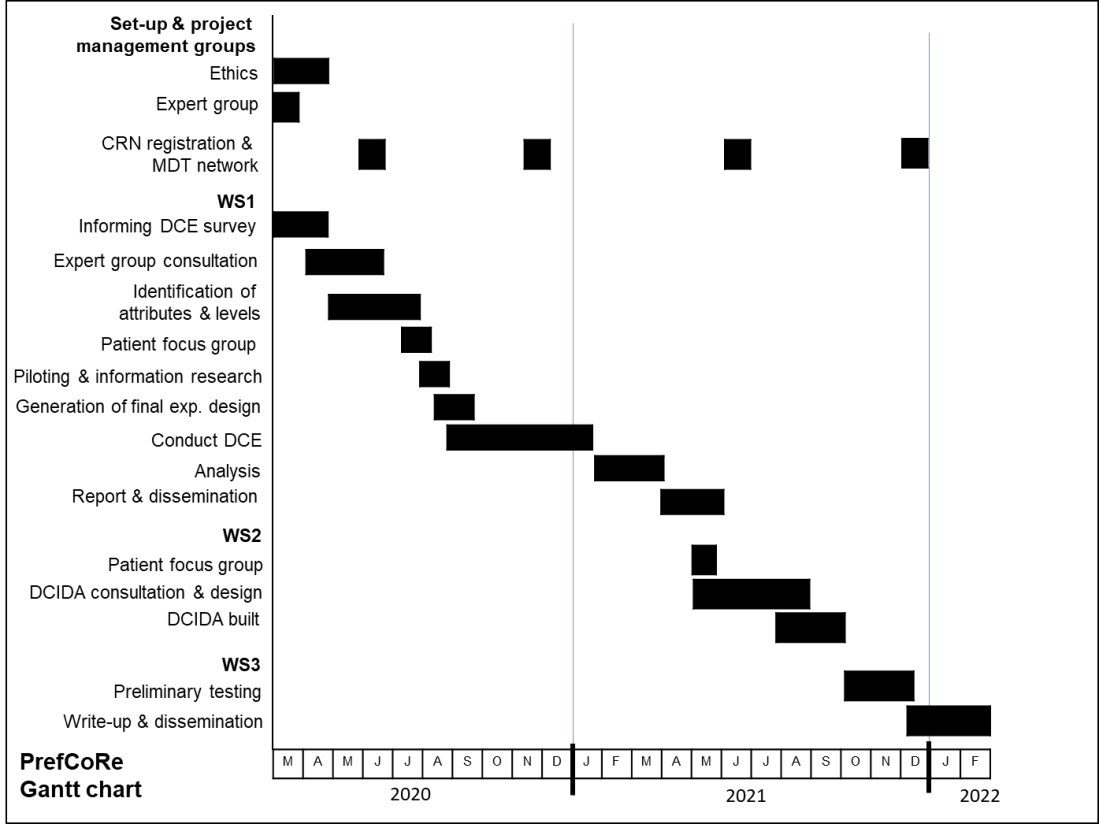
The following Gantt chart illustrates the three Work Streams (WS) and how the work will be carried out over the two years:
PPI: We conducted two online consultations with 48 people on treatment preferences. Results showed mixed views and the need for this research. We will consult patients and the public in the development of the survey and decision aid and in plans for dissemination of results. We are supported by the NIHR Manchester Biomedical Research Centre Patient and Public Involvement team.
Dissemination: The tool will be promoted via relevant major charities such as Bowel Research UK and Bowel Cancer UK. We are hugely grateful for the time and support provided by these charities who have made this project possible.
Funding: We are hugely grateful for the funding awarded by the NIHR Research for Patient Benefit (RfPB) Grant (Ref NIHR200500). For further funding information, please Click here.
Participant Information Sheet: Please click here for the latest version of the Participant Information Sheet for those completing the DCE.
Team: This is a collaboration between a rectal cancer clinical team; health economists (investigators with expertise in building decision aids); patients and public.

